What it is?
Neuroma is a benign neoplasm that does not manifest itself in any way for a long time . Many may not even know about the presence of a tumor on the spine until the end of their days.
Neuromas are also called schwannomas due to the fact that a neoplasm is formed from Schwann cells. They are the main myelin sheath of all nerve fibers.
Neuromas look like round, dense tumors that are located in a capsule.
Picture of the course of the disease
For several years, the spinal neuroma is completely invisible. After all, the growth rate of such a benign formation is 1–2 mm annually . But there is a low risk of schwannoma into a malignant tumor, which will grow much faster.
Even benign tumors reach large sizes over time. Most patients are diagnosed with single nodes. If left untreated, they can grow up to 2–3 kg .
Neuromas do not pose a direct danger to humans. But due to their presence, the quality of life may noticeably deteriorate. After all, neoplasms compress structures related to the central nervous system. Most often, tumors form in the cervical and thoracic spine.
Classification
Spinal neuromas can be benign or malignant . To determine the type, the patient must undergo a full examination.
Benign neuromas look like a round formation with clear boundaries. When examined over time, it is clear that it is growing slowly. In many patients, such neoplasms do not provoke the appearance of any disorders.
Malignant neuromas form as independent neoplasms or arise as a result of degeneration. They do not have clear boundaries, and the consistency is soft and elastic. They grow quickly. Malignant tumors can form metastases in other organs.
But benign schwannomas predominantly occur on the nerves of the spine. With prolonged growth and reaching large sizes, they can become malignant.
Depending on the location of dislocation, neuromas of the cervical, thoracic and lumbar regions are distinguished.
Prevalence
Neuromas are most often detected in women in middle and old age. In other categories of patients they occur much less frequently. Among all tumor diseases of the spine, neuromas account for 20%.
Risk factors, causes
Doctors have not yet been able to find out the reasons why Schwann cells begin to actively grow. It is only known that this pathology develops due to mutation of genes located on chromosome 22.
Researchers identify certain risk factors, under the influence of which there is a likelihood of developing pathology.
Most often, doctors call such provoking factors:
- influence of radiation;
- contact with various chemicals for a long time;
- hereditary predisposition to the appearance of tumors;
- neurofibromatosis;
- presence of other tumors;
- traumatic lesions of nerve endings.
The probability of developing neuroma in the presence of this disease in one of the parents is 50%, in two parents – 66.7%.
Consequences
The effect of schwannomas on human health depends on the location of the tumor and its size . With spinal neuromas, paresis and paralysis may develop. They appear due to compression of the spinal cord structures by the growing tumor.
If the degree of compression is small, then paresis appears . This is a neurological syndrome characterized by a weakening of voluntary movements of the limbs, they become noticeably weaker. Muscle rigidity and the appearance of trophic changes are observed.
With intense compression, complete paralysis occurs. The patient cannot move his limbs.
Paresis and paralysis can affect both one side (monoparesis, monoplegia) and 2 simultaneously (paraplegia, paraparesis).
Video: “Spine tumors”
Reasons for the development of neuroma
This disease is often called schwannoma in the medical literature. This is due to the fact that the abnormal formation grows precisely from the Schwann cells of the membrane. Scientists have not yet identified the main root cause of pathological cell division. Provoking factors are:
- exposure to radioactive background;
- low eco-level of the area of residence;
- systematic attack on the body of carcinogenic nutrients;
- poor air quality;
- hereditary predisposition;
- frequent, long-term inflammatory processes, infections.
Visually, the neoplasm is a tumor object enclosed in a membrane bounding it with an uneven, bumpy surface. The inner part is a gray or brown mass of cells with capsule-shaped inclusions filled with a liquid substance. The chemical composition is identical to the intracystic fluid. Due to the unlimited division of schwannomas, the object constantly grows, which leads to compression of adjacent tissues and nerve atrophy. The more limited the space in which the neuroma originated, the more pronounced the symptoms of the disease. The vascular network surrounds only the outer part of the tumor; the inner area is poorly nourished, which leads to degeneration of this area.
Symptoms and diagnostic methods
Neuromas are located mainly outside the spinal cord , they surround it. In the early stages, there are no signs of the disease, but as the tumor grows, several symptoms appear simultaneously.
The main signs of the appearance of neuroma include:
- pain radicular syndrome;
- the appearance of vegetative disorders;
- the occurrence of spinal transverse lesion syndrome.
With the development of radicular syndrome, patients begin to complain not only of pain in the area where the tumor grows. Pain can spread to different parts of the spine and other parts of the body. They intensify if the patient is in a horizontal position and weaken in a vertical position.
The severity and nature of the manifestation of radicular syndrome is directly related to which nerve was affected. The anterior roots control movement. If they are affected, paralysis of certain nerve fibers occurs. If a neuroma affects the dorsal roots, pain appears and sensitivity is impaired.
Patients complain about:
- sensation of warmth, cold;
- feeling of crawling sensations;
- numbness.
Discomfort is concentrated in the area that is innervated by the corresponding nerve plexus. With neuromas in the cervical region, pain occurs in the occipital region, and may bother the shoulders and neck.
If the schwannoma is located in the thoracic region , then the pain radiates to the arms, chest, and between the shoulder blades. The sensations are similar to those that occur with angina pectoris. The pain is localized in the chest area, radiating to the shoulder blade and arm.
Thoracic neuroma leads to disturbances in cardiovascular activity (the frequency of contractions decreases, cardiac conduction deteriorates), and the appearance of pain in the pancreas and stomach.
With schwannomas of the lumbar region, weakness, a feeling of stiffness in the legs appears, and strength decreases. Also, loss of sensation and pain may occur in the lower abdomen.
Neuroma in the lower back can cause problems with urination and defecation. Men experience erectile dysfunction.
If the cervical spine is affected , breathing problems appear, and sometimes swallowing function is impaired. Some patients even experience increased blood pressure.
When the spinal cord is damaged, spastic paralysis or paresis develops on the side where the neuroma is localized. On the opposite side, pain and temperature sensitivity is lost.
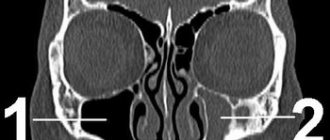
To identify a neuroma, after collecting an anamnesis and conducting a neurological examination, radiography, computed tomography or magnetic resonance imaging are prescribed. These are the main diagnostic methods.
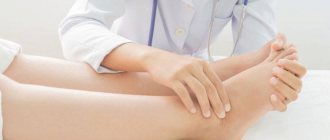
Diagnosis of Morton's neuroma
The diagnosis of Morton's neuroma is usually made based on patient complaints and examination.
The examination consists of provoking symptoms of Morton's neuroma. That is, the doctor tries to compress the nerve between the metatarsal bones by squeezing the foot with a hand. If the nerve is thickened and inflamed, then within 30-60 seconds the patient begins to experience numbness and a burning sensation in the 3rd interdigital space. This way the diagnosis is confirmed.
X-rays or MRI are performed to exclude other pathologies (consequences of trauma, osteoblastoclastoma and other tumors and soft tissue diseases).
Treatment
Did you know that...
Next fact
To get rid of neuroma, depending on its size, location and accompanying symptoms, the following treatment methods are prescribed :
- conservative;
- surgical;
- radiosurgery.
The doctor should determine the tactics of therapy.
Do you want to know what other spinal tumors there are?
- Why is spinal hemangioma dangerous for adults and what is it?
- To find out how syringomyelia is treated, go to page
- You can learn about the causes of cysts in the spine here
- You can study the consequences of developing a coccyx cyst in the following article
- You can find out what a perineural cyst of the spine is by following this link
- You can read about the median and lateral cervical cyst on the page
- How does spinal cancer manifest at an early stage?
Drugs
When treating with conservative methods, the emphasis is on the need to relieve the patient of pain, reduce the rate of tumor growth and eliminate other associated symptoms.
Conservative treatment is acceptable at an early stage of the disease or in cases where surgery is undesirable. Special agents are prescribed to slow down the growth of tumors.
The doctor may prescribe:
- diuretics (Mannitol);
- muscle relaxants (Sirdalud, Mydocalm);
- corticosteroids (Prednisolone).
The list of mandatory recommendations includes reducing the amount of salt and fluid consumed and maintaining water and electrolyte balance.
Surgery
Most often, patients are recommended to have neuromas removed immediately after they are identified. The doctor may recommend a conventional operation in which the neuroma and capsule are removed, radio wave therapy, CyberKnife .
In a conventional surgical procedure, the tissue is cut and the neuroma in the membrane is pulled out (if it is small) . The operation is performed using endoscopic instruments.
For large tumors, the capsule is first dissected and the neuroma is removed.
After this, the shell is carefully separated from the surrounding tissue and removed.
In some cases, doctors choose to use radio wave surgery .
This removal method is used only in situations where the size of the formation is no more than 3 cm.
It is used when there are contraindications to surgery. The problem area is treated with an ionizing emitter, under the influence of which all atypical cells die.
Video: “Laser removal of a spinal cord tumor”
Exercise therapy and massage
After a successful operation, the doctor may prescribe exercise therapy. Performing exercises helps stimulate the healing process. The likelihood of relapse with a proper rehabilitation period is reduced.
It is impossible to stop the growth of a tumor, get rid of pain and other symptoms with the help of exercise therapy or massage.
Treatment at home
If you feel pain or numbness, self-medication is pointless . Even procedures prescribed by a doctor in the form of injections of anti-inflammatory drugs and muscle relaxants will not help.
If a neuroma was discovered accidentally while no unpleasant symptoms arose, conservative treatment is possible. In other cases, surgery is needed.
Acoustic neuromas. Myths and reality
Radiology Tags:
Y. Titova:
Hello, the MediaDoctor channel and the program “Neurosurgery with Dr. Ilyalov” are on air. In the studio I am Yulia Titova, and the author and main presenter of this program is Sergei Ilyalov, a neurosurgeon, radiosurgeon. Hello, Sergey.
S. Ilyalov:
Good evening.
Y. Titova:
Today we will talk about acoustic neuromas, dispel myths and tell you about the real situation. But first of all, what is an acoustic neuroma?
S. Ilyalov:
Yulia, let me take a moment and congratulate you, your radio station in your person, on the first anniversary of your work, and wish you further success.
Y. Titova:
Thank you.
S. Ilyalov:
As for neuromas, they are benign tumors growing from the vestibulocochlear nerve sheaths. In other words, from the sheaths of the auditory nerve, which also has a vestibular portion. But most often this tumor originates from the vestibular portion of the auditory nerve. This tumor is notable in that it is one of the most common benign brain tumors in adults. And among tumors of the posterior cranial fossa, where the cerebellum is located, this is the most common benign tumor.
Y. Titova:
Is the nature of this disease clear today? What causes it?
S. Ilyalov:
The nature is clear; it is based on certain mutations that arise in the vast majority of patients over the course of life under the influence of certain external factors. We don’t know which ones exactly, but we know that there are quite a lot of harmful influences around, starting with solar radiation, electromagnetic radiation, and so on.
Y. Titova:
Is it possible to identify risk groups or people who are in this group? What factors are the most striking?
S. Ilyalov:
Reliable risk factors for the occurrence of neuromas have not been identified, but it can be assumed that patients who are often in conditions of increased noise may be prone to this. Of course, patients with neurofibromatosis are at risk for developing neuromas; this is an inherited disease.
Y. Titova:
You said that adults most often encounter neuromas. Why? Does this disease occur in young people or children?
S. Ilyalov:
In children, this disease most often occurs as one of the manifestations of neurofibromatosis, that is, an inherited disease in which not only the auditory nerves are affected, on both sides, but also benign tumors of the meninges, spinal cord, spinal cord roots and etc.
Y. Titova:
One of the first negative effects that comes to mind is frequent listening to loud music. Could this trigger the development of neuroma?
S. Ilyalov:
Let me emphasize once again that no reliable connection has been established between listening to loud music and the occurrence of neuromas. In the same way, a direct connection has not been established between the frequent use of mobile phones and the occurrence of certain benign or malignant brain tumors.
A reliable connection between listening to loud music and the occurrence of neuromas has not been established. In the same way, a direct connection has not been established between the frequent use of mobile phones and the occurrence of certain benign or malignant brain tumors.
Y. Titova:
This is a very scary story, because we often sleep together with our phones.
S. Ilyalov:
There are a lot of rumors about this, and information periodically appears when either American or British specialists establish something. But I haven’t seen any reliable information.
Y. Titova:
What does it mean about the development of this disease, where does it all begin?
S. Ilyalov:
Considering that neuromas originate from the vestibular portion of the auditory nerve, that is, from the portion that is responsible for conducting vestibular impulses, one of the most common symptoms is dizziness, which occurs periodically. They can be frequent, rare, strong or not very intense. Another symptom is the symptom of irritation of the auditory fibers. First of all, in the form of the appearance of subjective ear noise.
Y. Titova:
What does this noise sound like?
S. Ilyalov:
It can be of different intensity, different tonality, it can be a constant squeak or low-intensity noise. Many patients are quite bothered by this symptom, and this is the first complaint with which they turn to doctors.
Y. Titova:
Unfortunately, dizziness can be a symptom of many diseases.
S. Ilyalov:
Yes, definitely.
Y. Titova:
But then we must look holistically. That is, this is dizziness plus...
S. Ilyalov:
Certainly.
Y. Titova:
What can indifference to these symptoms lead to, what serious development?
S. Ilyalov:
I would like to continue about the symptoms. Considering that the auditory nerve is affected, another of the most common symptoms is some degree of hearing loss, which patients sometimes do not pay attention to when the decrease occurs very slowly. And only under certain circumstances do patients suddenly notice that they are, say, listening to a TV or radio program with their good ear turned toward the sound source. Sometimes it happens that hearing decreases quite quickly. And for patients this is a serious reason to see a doctor.
Y. Titova:
Let’s take older people, old people; they probably perceive these symptoms as a given, as a matter of course due to their age. But if this is still the neuroma we are talking about, what can it lead to?
S. Ilyalov:
Not only patients, but even doctors are not alert to the possible development of neuroma. And sometimes these patients can undergo certain conservative medicinal procedures for years for the so-called sensorineural hearing loss, which, in fact, is based on a tumor. But they are treated conservatively with various kinds of vascular drugs and vitamins, which can affect the acceleration of the growth of these tumors.
Y. Titova:
While preparing for the broadcast, I read that when people suddenly get up from a bed or chair, they can simply fall over and get lost in space. So, does this already indicate a serious development of the disease or not yet?
S. Ilyalov:
Rather, it speaks of the degree of involvement of the vestibular apparatus, the degree of its suffering. The fact is that our vestibular apparatus is bilateral, that is, it is part of the inner ear on the right and left sides. As long as there are symptoms of irritation of the vestibular apparatus, this is manifested by dizziness and instability. But from the moment the function of the affected vestibular apparatus disappears, this symptom can go away, because the vestibular apparatus on the opposite side takes on this function compensatory.
Y. Titova:
As you have already said, this formation is benign. Interestingly, it is located in our brain. Does the course of the disease depend on the size of this neuroma? It probably compresses the tissues and vessels that are around it. What can its existence in our heads lead to?
S. Ilyalov:
There are many nuances, but the general principle of the development of the pathological effect of these tumors is that as the tumor grows, it first affects the adjacent structures, first of all, the auditory nerve itself, and then, as the size of the formation increases, pressure gradually forms on the others structures: on the root of the facial nerve, on the root of the trigeminal nerve, on the brain stem, which is located nearby, on the cerebellar hemisphere, the cerebellar peduncle, and so on. That is, on those structures, anatomical, normal, that are located nearby. As the pressure increases, the manifestations that we talked about may be joined by other symptoms, which already at the peak of their severity are manifested by symptoms of increased intracranial pressure, when intracranial pressure increases inside the cranial cavity due to the large tumor volume. This can already manifest itself as various kinds of headaches, in extreme cases, nausea and vomiting.
Y. Titova:
Is it possible to check yourself for the presence of this neoplasm?
S. Ilyalov:
Unfortunately, there are no self-diagnosis methods. The first thing patients should pay attention to is that if they have not had any symptoms, let's say their hearing has always been normal, and they notice that the hearing on one side is starting to decrease.
Y. Titova:
I'll interrupt you about the rumor so that I can figure it out right away. Does hearing occur in both ears or just one?
S. Ilyalov:
The fact is that neuroma in approximately 90% of cases is a one-sided tumor. In 5% of cases it is an accidental bilateral neuroma, in another 5% of cases it is a neuroma due to neurofibromatosis, which I have already mentioned. If we are talking about the most common situations with unilateral tumors, then yes, we are most often talking about unilateral hearing loss.
Neuroma in approximately 90% of cases is a unilateral tumor.
Y. Titova:
Let's say our future patient came to the doctor with complaints. What diagnostics will the doctor perform to detect this disease?
S. Ilyalov:
First of all, you need to contact an ENT doctor or an otolaryngologist. There is a particularly narrow specialization of otolaryngologists, the so-called otoneurologists, who, in addition to examining the ear, nose and throat, can conduct certain tests, vestibular tests, which help identify certain signs of damage to the vestibular apparatus, hearing aid and adjacent structures. But reliable signs can be identified only by neuroimaging, that is, by computer or magnetic resonance imaging.
Y. Titova:
Can a neuroma give off cysts from itself, that is, can it spread?
S. Ilyalov:
What is a cyst? A cyst is a cavity filled with some content. Neuromas quite often have both a dense structure and a cystic or mixed structure, when in the dense stroma of the tumor, due to small hemorrhages as they resolve, the blood remains completely filled with these blood breakdown products. We can see this both on MRI and during surgery, when surgeons open these cysts, removing their contents along with the bulk of the tumor.
Y. Titova:
And if neuromas were nevertheless diagnosed, do they immediately resort to surgical treatment or are there any alternative methods?
S. Ilyalov:
Today there are three main tactics. The first is traditional; for small tumors, the so-called “wait and watch” tactic is acceptable. Its essence lies in the fact that the patient, in the absence of any significant symptoms for him, is offered periodic magnetic resonance imaging or computed tomography in order to determine whether the tumor is growing or not. If signs of growth appear, questions about surgical treatment or radiosurgical treatment, for example, using a gamma knife, are resolved. The “wait and watch” tactic has traditionally been used by neurosurgeons due to the fact that surgical removal of the tumor was associated and still continues to be associated with fairly high risks of functional impairment, both complete loss of hearing in the affected ear and damage to the function of the facial nerve, which passes through the neighborhood, which manifests itself in the asymmetry of the work of the facial muscles - facial distortion.
In principle, talk that a tumor, a neuroma, having once appeared, may then not grow, has only a partial basis in reality. We can say that such a course of neuroma can most likely be expected in elderly or even senile people, when metabolic processes in the body are already at a fairly low level, and in the tumor, in particular. And such tumors, if they are detected in patients over 75 years of age, if they are small in size, up to a centimeter, let’s assume, then they can be monitored. If a small tumor is detected in a young patient, by and large, observation does not make much sense.
The fact is that somewhere in the late 90s, early 2000s, when neuroimaging in the form of computed tomography and magnetic tomography was actively developing, there were a large number of publications devoted to the observation of acoustic neuromas in the dynamics. In fact, they compared images at intervals of a year, two, three, etc. But they compared either by conventional visual comparison, or used for this purpose certain elements of tumor measurement on identical sections. And they didn’t seem to find any difference. This is where that rumor came from, that idea that these tumors might not grow or change for many years. But you need to understand that the measurement methods used in these studies had a very large degree of error. And in recent years, when it became possible to measure nonlinear tumor sizes, already measuring volume, it turned out that the percentage of false negative results in previous studies was quite high. Therefore, these tumors grow very slowly, and it can be very difficult to notice the difference over the course of a year.
But let me give you an example: if a tumor with a diameter of only 1 cm increases by a millimeter, this is within the error of measuring linear dimensions. And if the difference in volume is about 30%, then this will already be a significant difference. And you need to understand that in young and middle-aged patients these tumors will almost certainly grow.
Conversations that a neuroma, once it appears, may not grow, are only partly based in reality.
Y. Titova:
Can a neuroma survive to the point where it is no longer safe to remove it for human health?
S. Ilyalov:
Yes maybe. The fact is that the risks of surgical removal of these tumors increase as the tumor size increases. These risks are associated both with a direct impact on adjacent structures, again, the facial nerve, and with an impact on the brain stem, with the possible formation of hydrocephalus due to disruption of the normal outflow of cerebrospinal fluid.
There are cases, and still occur, when patients do not turn to specialists for too long and are admitted for surgical treatment with giant tumors, and these cases are quite complex in surgical practice from the point of view of both surgical treatment and subsequent resuscitation support in the postoperative period.
Y. Titova:
Here's what to do in such a difficult situation, what decisions do doctors make?
S. Ilyalov:
Let's start with the fact that the decision should be made by a qualified specialist, a qualified neurosurgeon with experience in the surgical treatment of such tumors. You need to understand that today the possibilities of normal, timely diagnosis have expanded significantly. Now there are a huge number of diagnostic centers, both public and private, well equipped. And, in principle, there are no problems with the timely diagnosis of these tumors at the stage when they do not threaten the patient’s life and, moreover, do not yet cause even any significant changes in the patient’s health.
Y. Titova:
I would like to look at the treatment methods in more detail, and let's start in order. Surgical treatment – when is it most effective, how is the operation performed?
S. Ilyalov:
I will allow myself to expand the answer to your question a little right away. The fact is that in addition to conservative observation, which makes sense only in cases where the patient has high risks or even contraindications to surgical treatment, there are two main methods. This is either surgical removal, a traditional method that ideally allows the entire tumor to be removed. But at the same time, surgical treatment is associated with certain risks of functional disorders, which I have already mentioned. These are hearing impairment, hearing loss, in a large number of cases from 50 to 80%, dysfunction of the facial nerve of varying degrees of severity, with different tumor sizes it can range from a few percent to 20-25%. And this is one of the most common and significant complications for patients. As well as various kinds of complications that can accompany the operation as a whole. These are the risks of anesthesia, and the postoperative period, and liquorrhea, and hemorrhages in the bed of the removed tumor. And today, global statistics on mortality during such operations fluctuate somewhere around 1%.
Y. Titova:
If we remove this tumor and everything goes well, will my hearing return after this operation?
S. Ilyalov:
If hearing is already lost, it will not return. Moreover, the risks of recurrence of the tumors themselves after total removal range from 5-7%.
If hearing is already lost, it will not return. Moreover, the risks of recurrence of the tumors themselves after total removal range from 5-7%.
Y. Titova:
And typically how long does it take?
S. Ilyalov:
This can be a fairly long period of time, measured in years. But for this, we must understand, based on control MRIs performed after surgical treatment, that the tumor was completely removed, and then the risk is minimal.
Y. Titova:
But we can still say that a person who has undergone surgery to remove a neuroma should be monitored more often. We should all see doctors, but in this case we need to do it much more often.
S. Ilyalov:
The fact is that surgical removal of a tumor, an acoustic neuroma, often ends with the deliberate leaving of small fragments of the tumor either on the brain stem or intimately connected to the facial nerve. The surgeon specifically leaves it in order to avoid dysfunction of these structures. And these small remnants are precisely the cause of relapse.
Y. Titova:
This is an interesting point. That is, often the tumor is not completely removed, but a piece is left?
S. Ilyalov:
Yes.
Y. Titova:
Let's talk about the next method. If we have told you everything about surgery, let’s talk about radiosurgery, which is much closer to you. What is its effectiveness, who is this method indicated for and who is contraindicated?
S. Ilyalov:
The radiosurgery method has a fundamental difference from surgery, and this difference lies in the fact that we do not remove the tumor. We irradiate it, irradiate it entirely, in such a way that the entire radiation load is delivered to the tumor, while minimizing radiation exposure to all nearby adjacent functional structures - the structures of the inner ear, the vestibular apparatus, the cochlea, the facial nerve, the brain stem, the cerebellum, and so on. . The radiosurgical method is highly effective. Relapses after radiosurgery occur in approximately 1-2% of cases. This is over an observation period of about 10 years.
The radiosurgical method is highly effective. Relapses after radiosurgery occur in approximately 1-2% of cases. This is over an observation period of about 10 years.
Y. Titova:
Excellent statistics.
S. Ilyalov:
Moreover, these statistics are quite similar between different clinics around the world. These are both foreign statistics and ours, Russian ones.
Y. Titova:
But it would seem that radiosurgery should be used in any case, because the numbers are good and give hope. But still, when is it not applicable or maybe the issue is something else?
S. Ilyalov:
There are situations where surgical treatment has an advantage over radiosurgery and vice versa. Radiosurgical treatment is good for small tumors; it is justified in a situation where the symptoms that bother the patient do not have a significant impact on the quality of his life. Suppose the hearing is reduced, but only slightly, dizziness is present, but the patient retains his ability to work. He not only serves himself, but he is also professionally active and so on. In this situation, radiosurgery allows you to influence the tumor, stopping its growth, in many cases maintaining the patient’s functional status, and returning him to an active life in a short time, literally a few days after treatment. At the same time, the risks of functional impairments, in particular those associated with hearing impairment and hearing loss, are significantly less than with surgery. We are talking not so much about hearing loss, but about the possibility of preserving the hearing that the patient had at the time of detection of the tumor at the time of treatment.
Statistics for facial nerve dysfunction differ significantly from surgical statistics and fluctuate somewhere around zero. This is an extremely rare complication for us now. And in this situation, radiosurgery certainly has an advantage. But in the case of large tumors, more than 3-3.5 cm, which roughly compress the brain stem, which lead to the development of hydrocephalus, and so on, surgery clearly remains the first choice.
And in this regard, it is worth mentioning another treatment tactic, which in recent years has become widespread abroad and is now being recognized in our country. This is a tactic of combined treatment of large acoustic neuromas, when the first stage is to remove the tumor, but partially remove it in order to eliminate only the compressive effect it has on adjacent structures in order to preserve the function of, say, the facial nerve. The remaining small fragments of the tumor are routinely irradiated with radiosurgery in the second stage.
Y. Titova:
Well, here's my current idea. Radiosurgery is most effective at a time when we caught an innocent person at the very beginning of its inception, when it has not yet caused any damage, when it has not brought the symptoms that bother the patient. But if there are already effects on the surrounding organs and tissues, then surgically.
S. Ilyalov:
This effect must not only be visible on MRI, it must manifest itself symptomatically, and these symptoms must be quite severe. In this situation, surgery will be clearly justified, and radiosurgery recedes into the background.
Y. Titova:
But does radiosurgery have negative consequences, maybe there are risks or situations when radiosurgery does not go very well?
S. Ilyalov:
Radiosurgery of neuromas in general and acoustic neuromas in particular, as the most common type of neuromas, has one feature. Neuromas tend to temporarily increase in size in response to training. Typically, these changes are visible on follow-up MRIs ranging from several months to one to two years after radiosurgery. You need to understand that this is not true tumor growth. This is a reversible reaction, it is expected. In some cases, approximately 2-3%, such an increase in size, especially when the tumor was initially rather large, can lead to a significant increase, intensification of symptoms, and the appearance of new symptoms. And such patients require careful monitoring, perhaps even more frequent control images. In other cases, we know this feature, we expect it and do not experience any particular concern about it. We inform all patients that this may happen.
Neuromas tend to temporarily increase in size in response to training..
Y. Titova:
This is correct and fair. Is it possible to perform radiosurgery in remote regions, or are such operations still performed there using a conservative method?
S. Ilyalov:
I will say this: both surgery and radiosurgery are equal methods of treatment. Either one way or another can influence this tumor. Which treatment method a particular doctor will choose, which treatment method the patient or his relatives will choose, depends, first of all, on their awareness and mastery of certain methods of treatment.
Of course, radiosurgical treatment in our country is even less accessible than traditional surgical removal. But, on the other hand, many neurosurgical centers still do not undertake to operate on these tumors due to the serious functional risks that occur during such operations. And they prefer to send such patients to specialized institutions, for example, to the Burdenko Institute of Neurosurgery.
Y. Titova:
When a neuroma or any neoplasm is diagnosed, even if it is benign, it is not very pleasant. And what scares me the most is surgical intervention, radiosurgery, especially when it is not at all clear what it is. The patient asks you a question: is it possible to cure this with pills or somehow maintain it in the state in which it is now, what will you answer?
S. Ilyalov:
Yes, such questions were asked, but quite rarely. There is not a single method of conservative treatment of these tumors that would allow one to reliably control their growth and, moreover, achieve their reverse development.
There is not a single method of conservative treatment of neuromas that would allow one to reliably control their growth and, moreover, achieve their reverse development.
Y. Titova:
Let's talk about a neuroma that has started, can it transform into a malignant tumor?
S. Ilyalov:
Malignant types of neuromas do occur, but this is an extremely rare development option. No more than two dozen similar observations have been described in the literature.
Y. Titova:
But are they possible, and what is the reason for this?
S. Ilyalov:
The risk factor for malignancy is, again, neurofibromatosis, as well as some extremely rare variants of mutations that randomly arise in such patients.
Y. Titova:
Do patients who have undergone surgery, and it went well, experience any restrictions in their lives? Are there any lifestyle recommendations from doctors?
S. Ilyalov:
From neurosurgical practice, first of all, what has partly been transferred to us in radiosurgery is to avoid taking various types of biostimulants, natural or medicinal. We consider natural ginseng tincture, Eleutherococcus, Chinese Schisandra, and B vitamins from medicinal preparations. That is, these are the drugs and substances that activate all metabolic processes, in particular, this can also affect the acceleration of tumor growth. Accordingly, after surgical treatment, if we assume the presence of even small, insignificant residual fragments, these restrictions are of fundamental importance.
You need to understand that after surgical removal, the remnants retain their biological activity, but after radiosurgery, when we irradiate the entire volume of the tumor, the ability of tumor cells to further grow is suppressed. Therefore, to date there is no reliable evidence that taking B vitamins after radiosurgery significantly increases the risk of relapse. We do not have such data. However, we recommend that patients avoid it if possible.
Y. Titova:
And if you take young people, young patients who have survived this disease. Do sports and an active lifestyle continue to accompany this person or are there any restrictions?
S. Ilyalov:
It all depends on the patient’s well-being. By and large, the patient has no categorical contraindications to an active lifestyle. One of the myths in the treatment of young patients is that surgeons do not recommend radiosurgery, citing the fact that the long-term consequences of using the same gamma knife have not been studied - what if this tumor becomes malignant. I want to say this again. To date, there is no reason to refuse radiosurgery to young patients. The long-term results of radiosurgical treatment, primarily with the use of a gamma knife, have already been studied quite well. There is a large number of scientific studies on large populations of patients, measured in hundreds, under a thousand patients, who are observed for a period of 8-10 or more years. And there is no evidence that these patients have a significantly increased risk of malignancy of these tumors. Those two dozen cases of identified malignant tumors are all that have been identified to date among almost 70,000 patients treated.
To date, there is no reason to refuse radiosurgery to young patients. The long-term results of radiosurgical treatment, primarily with the use of a gamma knife, have already been studied quite well.
Y. Titova:
At the beginning of the broadcast, you said that neuroma also happens in children, and, as a rule, this is a hereditary story. How are small children treated or are they not treated, but the same observational method?
S. Ilyalov:
There are two options for children. If a child has a family history of parents suffering from neurofibromatosis, and there is already early suspicion of the possible development of neurofibromatosis, the disease and hearing damage in such a child may not be detected early enough. And then there is an opportunity, among other things, to carry out radiosurgical treatment without resorting to surgery, in order to preserve such a child’s hearing.
In the majority of children, neurofibromatosis may not be diagnosed immediately, even if there are some skin signs, when parents simply do not pay attention to these symptoms, these manifestations. And one of the manifestations of the disease may be its already quite advanced course with signs of increased intracranial pressure, hydrocephalus, and so on, when a large tumor is detected that has to be removed only surgically.
Y. Titova:
Can a pediatrician notice the symptoms?
S. Ilyalov:
Yes, of course, first of all, we pay attention to the skin manifestations of neurofibromatosis; a classic example is café au lait spots.
Y. Titova:
Where to treat this disease, in Russia or abroad?
S. Ilyalov:
We have already touched upon this issue of where to get treatment. In my opinion, it is always a matter of trust in a particular specialist. Not even the clinic, and even more so the fact of crossing the border is not a guarantee of good treatment results. As for the opportunities that are available in Russia, today they are absolutely comparable to similar opportunities in most Western clinics.
Y. Titova:
Our airtime is coming to an end, Sergey, let's summarize our conversation today. What should you pay attention to regarding your health and this diagnosis, where to go, who to go to, and what to do next?
S. Ilyalov:
If you or one of your family and friends experiences unmotivated dizziness, unilateral hearing loss, persistent persistent noise in the ear, do not brush off these symptoms, do not put off visiting a doctor, but go to an ENT doctor or an otoneurologist for treatment. initial examination. In the future, on your own initiative or at the direction of a doctor, you must undergo magnetic resonance imaging. This is the most informative method for diagnosing neuromas, which allows you to remove most questions regarding the cause of these symptoms.
Y. Titova:
Can I contact you at the clinic?
S. Ilyalov:
Can.
Y. Titova:
Can. Maybe you can tell us about your practice in relation to these diseases? How often do people come with this diagnosis?
S. Ilyalov:
In general, acoustic neuromas in radiosurgical practice are perhaps the third most common after metastatic brain lesions and after tumors of the meninges. What is good about neuromas in our practice is that the result, the functional results we strive for, are very reproducible and pleasing, especially in comparison with surgical treatment. Therefore, if a patient is diagnosed with an acoustic neuroma, it would be good to obtain at least two opinions - the opinion of a neurosurgeon and the opinion of a radiosurgeon.
Y. Titova:
Sergey, thank you very much, our broadcast has come to an end. Dear friends, in our studio there was Sergei Ilyalov, a neurosurgeon, radiosurgeon, and I, Yulia Titova. And as we found out, the disease is very common, unfortunately. Please get examined, get your loved ones examined, send them to doctors and monitor your health. All the best.
S. Ilyalov:
Thank you.
Recovery prognosis
If a neuroma is detected in a timely manner, doctors give a favorable prognosis, provided that the patient agrees to removal of the tumor . If you do not refuse treatment, the likelihood of paresis and paralysis is reduced to a minimum.
Even if malignant neuromas are identified, there is a 37 to 65% chance that the patient will live more than 5 years. These types of tumors grow more slowly than other tumors. However, if there is no opportunity to remove schwannoma, then the prognosis is less optimistic.