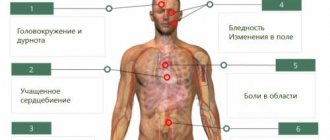
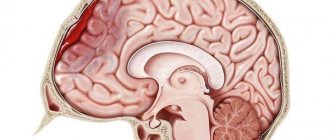
Features of the disease
Hemorrhages into the subarachnoid space (the gap between the meninges) occur spontaneously in most cases. The person then feels a sudden headache and nausea. Some people start vomiting, others lose consciousness.
Subarachnoid hemorrhage occurs due to complete rupture of blood vessels or partial tear of a cerebral artery . The reason for this is various pathological processes, most often aneurysms (protrusions of the walls of blood vessels) and traumatic lesions.
Blood accumulates in the area of the basal cisterns, so the disease can be called basal subarachnoid hemorrhage. Aneurysm ruptures cause blood to leak into the cerebrospinal fluid . In this case, a pronounced spasm of the arteries of the brain is observed, its edema develops, and neurons begin to die.
Prevalence of the disease and stages of its development
Among all forms of circulatory disorders in the brain, SAH occurs in 1-7% of cases . Spontaneous subarachnoid hemorrhage occurs in 8-12 people out of 100 thousand annually. Its traumatic form is more common. Depending on the situation, the frequency of subarachnoid hemorrhages in traumatic brain injuries varies from 8 to 59%.
Older patients are more likely to develop this condition. Alcohol intoxication is also a risk factor.
Almost 85% of cases occur due to rupture of the cerebral arteries, which are located in the circle of Willis. About half of subarachnoid hemorrhages are fatal. Of these, 15% of patients do not have time to get to the hospital .
There are 3 stages of development of traumatic subarachnoid hemorrhage.
- The blood that has entered the subarachnoid space begins to spread through the cerebrospinal fluid channels. In this case, the volume of cerebrospinal fluid increases and intracranial hypertension develops.
- In the cerebrospinal fluid, the blood begins to coagulate and clots form. They block the liquor pathways. As a result of this condition, liquor circulation is disrupted, and intracranial hypertension begins to increase.
- The dissolution of clotted blood is accompanied by the appearance of meningeal syndrome and signs of the onset of aseptic inflammation.
Parenchymal-subarachnoid hemorrhage
There are mixed forms of hemorrhagic strokes. One of these includes parenchymal-subarachnoid stroke. Its peculiarity lies in its focal symptoms. Depending on the structure affected, specific symptoms will be noted. For example, frontal symptoms with damage to the frontal lobe, visual impairment with damage to the occipital lobe, various types of apraxia and aphasia, impaired coordination and ataxia and other, more severe focal manifestations.
Important! In most cases, these symptoms will persist for life, although they may regress. Prolonged manifestation of focal symptoms is associated with compression or direct destruction of brain structures by the hematoma.
Classification of severity of conditions
Doctors use three methods to assess the severity of the lesion. When classified according to Hess and Hunt, 5 levels are distinguished :
- Asymptomatic or minor symptoms such as mild headache and neck stiffness. The survival rate for this condition is 70%.
- Moderate or severe pain, severe stiffness of the neck muscles, paresis of the nerves of the skull. The chances of survival do not exceed 60%.
- Neurological deficit in minimal manifestations, stunning. Only 50% of patients survive.
- Stuporous state, manifestations of moderate or severe hemiparesis, autonomic disorders, signs of decerebrate rigidity. The probability of survival does not exceed 20%.
- Agony, deep coma, decerebrate rigidity. In this condition, 90% of patients die.
The Fisher scale , modified by Claassen et al, is based on computed tomography findings. It distinguishes 4 degrees of damage:
- The first level is assigned when the hemorrhage is not visualized.
- We are talking about the second level in cases where the thickness of the lesion is less than 1 mm.
- At the third level, the thickness exceeds 1 mm.
- The fourth level of SAH is diagnosed in cases where intraventricular hemorrhages or their extension to the brain parenchyma are visualized, regardless of thickness.
The World Federation of Neurological Surgeons uses the Glasgow Coma Scale to assess focal neurological deficits:
- At level 1 there is no neurological deficit, GCS score is 15 points.
- To assign level 2 according to the GCS, there must be from 13 to 14 points and the absence of neurological deficit.
- If there are signs of damage to the central or peripheral nervous system and 13-14 points on the GCS, level 3 is established.
- The GCS score is 7-12; the presence of focal neurological deficit is not important.
- According to the GCS, less than 7 points were assigned.
Hemorrhagic stroke
Hemorrhagic stroke - hemorrhage in the brain and/or subarachnoid space, occurs four to five times less often than ischemic stroke
- Etiology of hemorrhagic stroke
The main etiological factors of hemorrhagic stroke are hypertension, arterial hypertension, congenital and acquired arterial and arteriovenous aneurysms. Subdural and epidural hematomas are usually of traumatic origin. Less commonly, the cause of hemorrhagic stroke can be hemorrhagic diathesis, the use of anticoagulants, amyloid angiopathies, mycoses, tumors, and encephalitis.
The predominant localization of hematomas is the cerebral hemispheres (about 90% of parenchymal hemorrhages); in 10% of cases, damage to the brain stem or cerebellum is detected. In most cases, there is a rupture of the vessel, much less often - diapedetic hemorrhages.
The clinic of parenchymal hemorrhages has general cerebral and focal symptoms. The clinical picture of subarachnoid hemorrhages includes two main groups of symptoms: cerebral and meningeal. In the presence of these and focal symptoms, we are talking about subarachnoid-parenchymal hemorrhage. Features of the clinical picture of parenchymal hemorrhages depend on the location of the hematoma.
- Hemorrhagic Stroke Clinic
Parenchymal hemorrhages. Hemorrhage into the putamen occurs with severe impairment of consciousness and a neurological defect in the form of contralateral hemiplegia, hemianesthesia, aphasia (with damage to the dominant hemisphere) or spatial hemiagnosia and anosognosia (with damage to the non-dominant hemisphere). The clinical picture is similar to that of middle cerebral artery occlusion.
With hemorrhages in the thalamus, as well as with hemorrhages in the putamen, herniation and coma are possible. Important signs of thalamic damage are greater severity of sensory disorders than motor ones, and unusual oculomotor disorders, often in the form of limited gaze, strabismus.
Table 1. HUNT Scale (Henry JM Barnett, Stroke, 1986) | |
| Degree | Characteristic |
| 0 | Unruptured aneurysm |
| I | Asymptomatic or minimal headache and mild neck stiffness |
| I.A. | Absence of meningeal or cerebral symptoms, but presence of persistent neurological deficit |
| II | Moderate to severe headache, stiff neck; no neurological deficit other than cranial nerve palsy |
| III | Drowsiness, confusion (disorientation in time and space), or mild local deficits |
| IV | Stupor, moderate to profound hemiparesis, possible early decerebrate rigidity and autonomic disturbances |
| V | Deep coma, decerebrate rigidity and signs of agony |
Hemorrhage into the pons is usually characterized by early development of coma, pinpoint pupils that do not respond to light, and bilateral decerebrate rigidity.
Hemorrhage into the cerebellum is characterized by sudden dizziness, vomiting in combination with severe ataxia, abasia, aesthesia and gaze paresis. Consciousness is not impaired, but compression of the trunk can lead to death.
Subarachnoid hemorrhage. Aneurysm rupture. Subarachnoid hemorrhage (SAH) is most often caused by the rupture of a saccular aneurysm, a defect in the internal elastic membrane of the arterial wall, usually occurring at the site of a bifurcation or branch of an artery. In most cases, the gap occurs between the ages of 35-65 years. There may be associated anomalies such as polycystic kidney disease or coarctation of the aorta. Sudden, unexplained headache of any location should raise suspicion of SAH and a computed tomography (CT) scan should be performed. For aneurysms larger than 7 mm, microsurgical obliteration is justified.
Another type of aneurysm is located along the internal carotid, vertebral or basilar artery; Depending on their structure, they are divided into fusiform, spherical and diffuse. Such aneurysms become clinically apparent when they put pressure on adjacent structures or due to thrombosis, but rarely rupture.
Table 2. Classes of social and everyday activity(Schmidt E.V., Makinsky T.A., Research Institute of Neurology, 1979) | |
| I | Return to work and complete independence from others |
| II | Return to work with limitations, independence in activities of daily living, walking without assistance |
| III | Limitation of previous household duties, partial dependence on others in everyday life, walking around the apartment without assistance, walking down the street with assistance |
| IV | The impossibility of returning patients who previously worked and suffered a stroke to work; for those who were engaged in housework, there is a significant limitation in the range of household duties or a complete inability to perform them, significant dependence on others in everyday life. Walking around the apartment with assistance. Sick people don't walk down the street |
| V | Complete loss of any productive activity. Complete dependence on others in everyday life |
A ruptured aneurysm is characterized by a sudden, intense headache. The patient usually says that he has never experienced such a severe headache before. Possible loss of consciousness; sometimes it turns into a coma, but more often consciousness is restored, although stupor remains. In some cases, loss of consciousness occurs suddenly, before the headache appears. SAH often occurs during exercise. When an aneurysm ruptures, the diagnosis is usually simple, but sometimes at an early stage there are no objective symptoms, so if there is a sudden headache, the doctor must think about subarachnoid hemorrhage.
Meningeal symptoms and low-grade fever are often present. Ophthalmoscopy often reveals subhyaloid hemorrhages.
Hemorrhage may be limited to the subarachnoid space or spread to the brain, causing focal symptoms. Sometimes, soon after hemorrhage, an ischemic stroke develops due to impaired blood flow or thrombosis in the arteries affected by the aneurysm.
It is not easy to determine the location of an aneurysm clinically, although it is sometimes possible. Thus, pain in the depths of the orbit and damage to the II-VI cranial nerves indicate an aneurysm of the cavernous part of the carotid artery; hemiplegia, aphasia and a number of other symptoms - for an aneurysm of the middle cerebral artery; damage to the third cranial nerve - an aneurysm at the junction of the posterior communicating and internal carotid arteries; abulia and weakness in the leg - due to an aneurysm of the anterior communicating artery; damage to the lower cranial nerves - an aneurysm of the basilar or vertebral artery.
A transient or persistent focal neurological defect that develops several days after a stroke is usually caused by a spasm of cerebral vessels that occurs in response to blood entering the subarachnoid space. Both an early and late complication of SAH can be hydrocephalus, which sometimes requires ventricular bypass.
Arteriovenous malformations. Arteriovenous malformations usually manifest as epileptic seizures or hemorrhage, but with large lesions, ischemia of adjacent areas of the brain may occur due to large blood flow. Most often this is a combined parenchymal-subarachnoid hemorrhage. People usually suffer from arteriovenous malformations in childhood and adolescence. That is why, for persistent headaches at this age, listening in the area of the orbit, carotid artery, and mastoid process is necessary.
The presence of vascular murmurs in these areas is pathognomonic. In doubtful cases, as well as for the purpose of differential diagnosis of telangiectasia and other angiomas, a CT scan can be done.
- Diagnosis of hemorrhagic stroke
CT is the method of choice. It allows not only to confirm the diagnosis, but also to determine the extent of the lesion in intracerebral parenchymal hemorrhages. CT is the best method for diagnosing SAH, and in most cases reveals blood in the subarachnoid space. This method also makes it possible to diagnose cerebral edema, parenchymal and intraventricular hemorrhage, and hydrocephalus. It is possible to identify the localization of the source in intrathecal hemorrhage.
Magnetic resonance imaging (MRI) compared to CT is more reliable in diagnosing small hematomas localized in the pons and medulla oblongata, as well as hematomas in which the X-ray density of blood clots inside is equal to the density of brain tissue. MRI also makes it possible to identify arteriovenous malformations that are accessible to surgical intervention, which are very difficult to diagnose with CT, especially without contrast enhancement.
Cerebrospinal fluid examination is indicated only in cases where computed tomography is not available. Blood in the cerebrospinal fluid is detected in all cases of SAH, as well as with hemorrhages in the cerebellum and pons; with minor hemorrhages in the putamen and thalamus, red blood cells may appear in the cerebrospinal fluid only after 2-3 days.
X-ray of the skull reveals calcified malformations and aneurysms. As a rule, it is not carried out.
Cerebral angiography is usually performed immediately before surgery to clarify the location and anatomical nature of the aneurysm, as well as to confirm the presence or absence of focal cerebral vagospasm. In severe cases, angiography is best performed only when the diagnosis is unclear and especially when surgical decompression is indicated.
- Differential diagnosis of strokes
Cerebral crises precede cerebral hemorrhage; the disease begins violently, suddenly, often during the day due to physical stress or excitement. Precursors are characteristic (flushing to the face, headache, seeing objects in red); prolonged comatose states develop (sometimes several days); the face is hyperemic; temperature rises; breathing is bubbling, hoarse; pulse intense, rare; accent of the second tone at the top; blood pressure is increased; miosis or mydriasis on the side of the lesion; focal symptoms are identified in the form of rapid development of hemiplegia with a decrease in muscle tone, reflexes, and skin temperature; sometimes epileptiform seizures or early contractures (tonic spasms, protective hyperreflexia) occur; pronounced meningeal phenomena, brainstem disorders (breathing disorders, vomiting, floating movements of the eyeballs); pseudobulbar reflexes are rarely detected, urinary retention or incontinence is observed; retinal hemorrhages are visible in the fundus; cerebrospinal fluid is hemorrhagic, xanthochromic, pressure is increased; leukocytosis in the blood, prothrombin is not increased; in the urine there are red blood cells, sometimes sugar and protein.
Ischemic thrombotic stroke is preceded by transient cerebrovascular accidents. The disease develops gradually, more often at night, in the morning or during sleep; there are warning signs (dizziness, short-term disturbances of consciousness); characterized by incomplete or short-term loss of consciousness; the patient's face is pale, the temperature usually does not rise; slow breathing, weak pulse; heart sounds are muffled; blood pressure is not elevated; the size of the pupils most often does not change; focal symptoms appear in the form of hemiplegia or monoplegia with low muscle tone, one-sided Babinski reflex; hemiplegia develops gradually and is unstable; epileptiform seizures are not typical; there are no meningeal phenomena; stem phenomena are rarely observed (with extensive foci); with repeated strokes, pseudobulbar reflexes occur; sometimes there is urinary incontinence; narrowing and unevenness of blood vessels are visible in the fundus; the cerebrospinal fluid is clear, the pressure is normal; hypercoagulation is detected in the blood; urine specific gravity is low.
Non-thrombotic ischemic stroke is preceded by crises, angina, myocardial infarction, etc.; the disease develops suddenly during the day, more often after physical activity; often without warning; characterized by short-term loss of consciousness, stupor; the face is pale; the temperature is elevated; weakened, slow breathing; pulse is arrhythmic, weakened; muffled heart sounds, sometimes atrial fibrillation; blood pressure is low, pupils are constricted; transient hemiplegia develops with mildly increased muscle tone and a one-sided Babinski reflex; epileptiform seizures are rare; meningeal and stem phenomena are rare; pseudobulbar reflexes are often detected; there is urinary incontinence; sclerosis and narrowing of retinal vessels are visible in the fundus; cerebrospinal fluid is clear, its pressure is sometimes increased; Prothrombin is increased in the blood, traces of protein are detected in the urine.
- Treatment of hemorrhagic stroke
General principles. Along with differentiated therapy for hemorrhagic stroke, basic therapy aimed at maintaining vital body functions plays an important role. The more severe the course of the stroke, the more necessary is multilateral and complex basic therapy, which is carried out individually, under the control of laboratory parameters and the functions of all organs and systems.
In connection with modern pathogenetic concepts, early diagnosis of cerebral stroke, clarification of its nature and organization of emergency medical care at the prehospital and hospital stages are of particular importance. The effectiveness of treatment measures depends on the timeliness of their initiation and on the continuity of therapy in all periods of the disease.
The continuity of treatment measures is determined by the general tactics of patient management and is associated with solving organizational problems: rapid transportation of the patient, clear organization of the work of the emergency department; early clarification of the diagnosis and resolution of the issue of referral to the appropriate department; smooth operation of all levels of assistance.
Neurosurgical intervention. The problem of hemorrhagic stroke, according to most researchers, is largely neurosurgical. If ischemic stroke is a process of development of hemodynamic and metabolic changes, ending mainly a few days after an acute cerebrovascular accident, then hemorrhagic stroke is a fait accompli of hemorrhage, and its pathogenesis involves secondary phenomena of already shed blood.
Removal of a hematoma after an intracerebral hemorrhage, if it is localized in an accessible area of the brain (for example, in the cerebellum, putamen, thalamus, or temporal lobe), can save the patient's life. The operation is indicated as early as possible (24-48 hours) for aneurysm ruptures, if the patient’s condition does not improve and signs of herniation appear. The main operation is clipping the neck of the aneurysm; wrapping the aneurysm with muscle or, less commonly, extracranial occlusion of the internal carotid artery is also performed.
Patients whose condition corresponds to grade 0 - III on the Hunt scale have no contraindications on this scale for hospitalization in the neurosurgical department (Table 1).
Differentiated conservative therapy. Conservative therapeutic interventions for hemorrhagic stroke should be aimed at rapid correction of blood pressure to optimal values for a particular patient; to combat developing cerebral edema and to carry out hemostatic and vascular wall-strengthening therapy.
Correction and control of blood pressure. If possible, blood pressure (BP) should be avoided. They try to keep the blood pressure within normal limits using antihypertensive drugs (beta blockers, calcium antagonists, antispasmodics, ACE inhibitors). To prevent emotional reactions, sedative therapy (diazepam, elenium) is prescribed. Sometimes phenobarbital is prescribed for prophylactic purposes (30 mg orally three times a day), since it also has an anticonvulsant effect.
To avoid straining, laxatives (regulax, glaxena, senade, etc.) are prescribed. It is necessary to create conditions for “protective inhibition”; protect from light and noise.
Hemostatic therapy and therapy aimed at strengthening the vascular wall. Prescribe dicinone (sodium ethmazilate) intravenously or intramuscularly (250 mg four times a day); antiprotease drugs for 5-10 days: gordox (100 thousand units four times a day intravenously) or contrical (30 thousand units immediately, and then 10 thousand units twice a day intravenously).
Calcium preparations (calcium pantothenate, berrocca, calcium gluconate - i.m., calcium chloride - i.v.), rutin, vikasol, ascorbic acid strengthen the vascular wall well.
Antifibrinolytic therapy in the form of gamma-aminocaproic acid up to 30 g per day (100-150 ml of a 5% solution intravenously, then orally) is of great importance. It can be administered with small doses of rheopolyglucin, which improves microcirculation.
Fighting cerebral edema. If lethargy or signs of herniation appear, it is better to prescribe osmotic diuretics mannitol (0.5 - 1.5 g/kg of the patient’s body weight, IV) or glycerin (1 g/kg orally). Less commonly prescribed corticosteroids are dexazone according to the scheme (8+4+4+4 mg IV). More effective are Lasix (20 mg IV twice a day) and/or Reogluman (200 ml IV drip twice a day).
Treatment of spasm of cerebral vessels. Signs of cerebral vasospasm (drowsiness, focal symptoms) appear after two to three days and most often on the seventh day after a hemorrhagic stroke. It is believed to be caused by the release of serotonin, catecholamines, peptides and other vasoactive substances. Prescribed for spasms, and even better for preventive purposes in advance. Calcium antagonists - nimoton (10 mg IV drip) - 10-14 days or nimodipine (30-60 mg orally every four hours). In this case, correction of antihypertensive therapy is necessary, since calcium antagonists affect blood pressure.
Rehabilitation treatment. Rehabilitation therapy is carried out over a long period of time and at all stages of treatment, but it is especially important after the acute period of a stroke. Physiotherapy exercises are combined with physiotherapy, acupressure and classical massage, acupuncture, electrical stimulation, and magnetotherapy.
Occupational therapy is required - training in self-care skills, work on training stands and work simulators. Psychotherapy is effective: individual, group, family; Autogenic, adaptive training, etc. are recommended. Speech therapy classes are required for persons with speech impairments.
The patient needs treatment for a total of at least three to four months. For severe strokes, depending on the patient’s condition, this period can be extended to six months or more. Patients are registered at the dispensary. With a prolonged period of restoration of functions, patients are transferred to disability.
- Work ability examination
Currently, there are five classes of social and everyday activity (Table 2).
The disability group is determined according to the severity of dysfunction and profession. Patients with paralysis of the limbs and aphasia need care from outsiders and are recognized as group I disabled people. In case of deep paresis, when the ability to self-care remains, but the ability to work is lost, disability group II is assigned. Group II patients adapt to working from home: typing, assembling parts, doing dispatch activities on the phone, etc.
Literature
1. Bogolepov N.K. Clinical lectures on neurology, 1971. 2. Internal diseases. Ed. Harrison T. R., vol. 10, 1997. 3. Gusev E. I., Skvortsova V. I., Chekneva N. S. et al. Treatment of acute cerebral stroke (diagnostic and therapeutic algorithms), M., 1997. 4. Allen GS, et al. Cerebral arterial spasm: A controlled trial of nimodipine in patients with subarachnoid hemorrage. //N. Engl. J. Med. 308:619, 1983. 5. Cerebral embolism study group. Brain hemorrhage and management options. Stroke 15:779, 1984. 6. Curling OD et al. An analysis of natural history of cavernosus angiomas. J Neurosurgery 75:702, 1991. 7. Henry JM, Barnett. Stroke: Pathophysiology, Diagnosis, Management. 1986. 8. Manual of Neurologic Therapeutics. Edited by Martin A. Samuels, MD 1995. 9. Nibbelink DW, Torner JC, Henderson WG Interactional aneurysms and subarachnoid hemorrage: A cooperative study. Antifibrinolytic therapy in recent onset subarachnoid hemorrhage. Stroke 6:662, 1975. 10. Origitano TC et al. Sustained increased cerebral blood flow with prophylactic hypertensive hypervolemic hemodilution (“Triple-H Therapy”) after subarachnoid hemorrage. Neurosurgery 27:729, 1990. 11. Wilkins RH Natural History of Intracranial Vascular Information: A review. Neurosurg 16:421, 1985.
Causes and risk factors
SAH occurs due to disruptions in the integrity of the walls of the arteries that run inside the skull. They are located on top of the hemispheres of the brain or at its base. The following are the causes of arterial damage:
- traumatic lesions: traumatic brain injuries, in which brain contusion and arterial damage are diagnosed;
- spontaneous violations of the integrity of the walls;
- aneurysm ruptures;
- ruptures of arteriovenous malformations.
In most cases, non-traumatic subarachnoid hemorrhage occurs due to the sudden rupture of an aneurysm in the arteries of the brain.
Experts include the following risk factors:
- use of alcohol and drugs;
- high blood pressure;
- vascular atherosclerosis;
- infections that damage the cerebral arteries (syphilis).
What diseases can it be associated with?
Diseases in which the development of subarachnoid hemorrhage is possible are represented by the following:
- primary vascular diseases of the central nervous system:
- arterial aneurysms of cerebral vessels;
- vascular malformations of the central nervous system
- arteriovenous malformations,
- cavernomas,
- arteriovenous fistulas;
- Nishimoto disease,
- dissecting aneurysms of cerebral vessels.
- arterial hypertension;
- vasculitis;
- blood diseases;
- violation of the blood coagulation system (as a result of taking anticoagulants, antiplatelet agents and other drugs).
Clinic: symptoms and signs
It is necessary to call an ambulance for subarachnoid hemorrhage if, against the background of normal health, a person has:
- headache that gets worse with any activity;
- nausea and vomiting;
- the appearance of psycho-emotional disorders: fear, drowsiness, increased excitability;
- convulsions;
- disturbance of consciousness: stupor, fainting or coma appears;
- the temperature increased to febrile and subfebrile values;
- photophobia.
Symptoms persist for several days.
Separately, there are signs that arise when the functioning of the cortex and nerves of the brain is disrupted . This is evidenced by:
- loss of skin sensitivity;
- speech problems;
- the appearance of strabismus.
A few hours after the effusion of blood, symptoms of meningitis appear:
- Kernig's sign (a person is unable to straighten a leg that is bent at the same time at the knee and hip joints);
- stiffness of the neck muscles (the patient does not reach his chin to his neck).
Traumatic subarachnoid hemorrhage due to traumatic brain injury requires monitoring for signs of damage to different brain regions.
Problems with the frontal lobe will be indicated by:
- speech disorder;
- cramps in the fingers;
- unsteady gait;
- speech disorders;
- behavior changes.
When the temporal lobe , hearing is lost, memory impairment, auditory hallucinations and tinnitus appear.
Impaired reading ability, loss of tactile sensations, and ability to navigate indicate problems in the parietal lobe .
Damage to the occipital lobe results in visual impairment and visual hallucinations.
With a relapse, existing symptoms intensify and new ones appear. For some, blood pressure rises, arrhythmia begins, pulmonary edema occurs and the heart stops.
Diagnostics and first aid
The doctor assesses the patient's condition and prescribes a computed tomography scan. Using CT:
- the area where the bleeding occurred is identified;
- data on the liquor system is obtained;
- it is checked whether there is cerebral edema.
High-precision CT angiography allows you to find out where the source of bleeding is . Negative CT results are associated with insignificant amounts of hemorrhage. They also occur when diagnostics are carried out at a later date.
If negative results are obtained, a lumbar puncture and cerebrospinal fluid examination are prescribed. SAH is indicated by an increasing concentration of red blood cells.
If the disease occurs due to an aneurysm, then vascular angiography . A radiopaque contrast agent is injected into them and X-rays are taken. Endovascular surgery is performed on damaged areas.
First aid is aimed at stabilizing the patient's condition. He needs to be taken to the hospital when the first symptoms appear .
Treatment is carried out to stop the bleeding and eliminate its source. It is important to prevent the development of complications and relapses.
Treatment tactics
Patients with SAH are immediately prescribed medications that normalize intracranial and blood pressure . If the patient is unconscious, then the trachea is intubated and a ventilator is connected.
People with massive hemorrhages undergo emergency surgery to remove the hemorrhagic contents . The rest are receiving therapy that should reduce the risk of recurrent bleeding.
The doctor faces the following tasks:
- achieve stabilization of the condition;
- prevent relapses;
- normalize homeostasis;
- minimize the manifestations of the disease that led to the lesion;
- treat and prevent vascular spasms and cerebral ischemia.
Patients are given pain relief using means that provide minimal sedation.
This allows you to control their consciousness. Checking water balance and assessing kidney function is carried out using a urinary catheter. People with SAH are fed using a nasogastric tube or parenterally. Compression garments help prevent vein thrombosis.
If the cause of the disease is an aneurysm, then during angiography the problematic vessel may be clipped or clogged .
is also carried out :
- patients who experience seizures are prescribed anticonvulsants;
- people with cerebral edema are given diuretics;
- for repeated vomiting, give antiemetics.
Treatment of other diseases starting with the letter - s
| Treatment of salmonellosis |
| Treatment of cutaneous sarcoidosis |
| Treatment of pulmonary sarcoidosis |
| Treatment of Kaposi's sarcoma |
| Treatment of uterine sarcoma |
| Treatment of Ewing's sarcoma |
| Treatment of type 2 diabetes mellitus |
| Treatment of type 1 diabetes mellitus |
| Treatment of seborrhea |
| Treatment of sepsis |
| Treatment of heart failure |
| Treatment of anthrax |
| Treatment of Budd-Chiari syndrome |
| Treatment of Guillain-Barré syndrome |
| Treatment of Gilbert's syndrome |
| Treatment of Parhon's syndrome |
| Treatment of polycystic ovary syndrome |
| Treatment of empty sella syndrome |
| Treatment of irritable bowel syndrome |
| Treatment of Sjögren's syndrome |
| Treatment of sinusitis |
| Treatment of systemic lupus erythematosus |
| Treatment of systemic scleroderma |
| Treatment of systemic sclerosis |
| Treatment of syphilis |
| Treatment of scoliosis |
| Treatment of somatoform disorders |
| Treatment of spinal stroke |
| Treatment of spondylosis and spondyloarthrosis |
| Treatment of laryngeal stenosis |
| Treatment of tracheal stenosis |
| Treatment of stenosing ligamentitis |
| Treatment of tetanus |
| Treatment of stomatitis |
| Treatment of ringworm |
| Treatment of subdural hematoma |
The information is for educational purposes only. Do not self-medicate; For all questions regarding the definition of the disease and methods of its treatment, consult your doctor. EUROLAB is not responsible for the consequences caused by the use of information posted on the portal.
Expected prognosis and possible complications
The consequences of subarachnoid hemorrhage in the brain depend on the reasons that caused it, how quickly the patient was hospitalized, and how adequate the treatment was. The prognosis is influenced by the age of the patient and the amount of bleeding.
The most serious complication of subarachnoid cerebral hemorrhage is vasospasm. This vasospasm leads to ischemic brain damage. In severe cases, death is possible. Delayed ischemia occurs in 1/3 of patients , half of whom experience irreversible neurological deficit.
The development of vasospasm can be prevented by the introduction of calcium channel blockers. But for traumatic lesions such drugs are not used.
There are other consequences:
- Relapse. It happens both in the early period and after a certain period of time.
- Hydrocephalus - cerebrospinal fluid accumulates in the ventricles of the brain. Occurs in early and late periods.
- Pulmonary edema, ulcerative bleeding, myocardial infarction. These complications occur rarely.
Among the long-term consequences are:
- attention disorder;
- memory problems;
- fatigue;
- psychoemotional disorders.
People after SAH often complain of headaches, and sometimes pituitary and hypothalamic hormonal regulation is disrupted.